Author’s Note: This is a repost of an article on my old blog that I wrote in March 2020.
A couple of weeks ago, I enrolled in an online course named “Lessons from Ebola: Preventing the Next Pandemic” from Harvard University in hope of gaining a more educated standpoint on how to deal with the current COVID-19 situation.
In this post, I’ll combine what I’ve learned in the course with my own research and observations into lessons applicable to COVID-19 in 5 sections: 1) A comparison of COVID-19 to Ebola, the most recent pandemic; 2) Trust and Community Engagement as essential elements for success in the fight against pandemics; 3) What you can do as an individual to fight COVID-19; 4) What nations can do to fight COVID-19 and 5) Helpful Resources. Feel free to read all or skip to the sections that interest you the most.
1. “Not enough people die from Corona for it to be dangerous! Ebola’s death rate was way higher!”
Opening up the long post, let’s talk about how COVID-19 has been continually compared to past epidemics and how these comparisons seem to make sense, but really don’t. With the overall mortality rate of COVID-19 at only 4% compared to the double digits of its predecessors, many people—like the young man below—are skeptical of whether it’s really that dangerous at all.

The tweet then follows with a specific comparison of COVID-19′s then 3.4% mortality rate to the 2014 outbreak of Ebola’s 50% mortality rate in attempt to downplay COVID-19′s dangers and justify OP’s “you only live once” mentality.
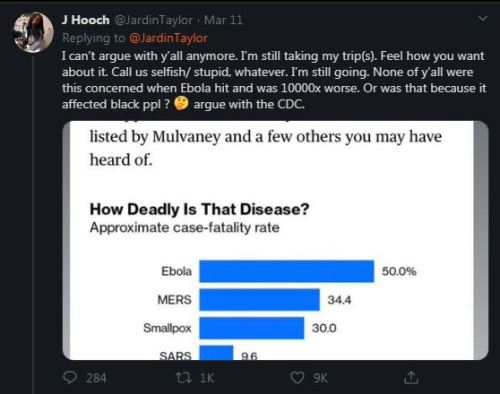
Looking at this gap, COVID-19′s dangers couldn’t possibly compare to past outbreaks, right? Well… not quite. While the statistics are correct, the way they’re used here completely disregards other important factors regarding the context of how these diseases are spread, making it hard to compare whether one is “more dangerous” than the other at all.
If you really want to compare, you need a holistic comparison of the contexts, resources available, responses and much more. I’ll give a few examples below to show how the two epidemics are different:
A. International and Local Response
In case of the 2014 Ebola epidemic, WHO took extremely long to declare the situation an international emergency. The first Ebola cases hit in December 2013, but only 8 months later did WHO announce “emergency” status. By then, with no funds/aid to buy medical equipment and no volunteer health workers mobilized to aid the severe lack of doctors on site, the damage done was already too great. More than half of the 2500 patients had already lost their lives. With no resources and no international help in those entire 8 months, local governments struggled immensely, resulting in responses so weak that many citizens lost faith in the system. This meant there was no unanimous cooperation to fight Ebola in the beginning.
With COVID-19, WHO’s pandemic warning came much faster: less than 4 months after the first case in November 2019. This means that countries will have more time to prepare themselves in advance before the virus reaches its peak in their own lands, and that funding/aid can be efficiently funneled to places currently that need them the most. In China, where COVID-19 first appeared, the government were incredibly robust in responding to the crisis, immediately locking down the region, mobilizing resources and educating their people. Unlike the West Africans with Ebola, the Chinese had trusted their governments and been highly involved in the fight against corona since the beginning. It only took China 2 months to shut down schools, whereas it took the West Africas 6-7 months. For the Ebola epidemic, these delays dealt a fatal blow to their already sky-high number of casualties.
B. Resources Available in Countries of Breakout
In Sierra Leone, Guinea and Liberia where most cases of Ebola broke out, there were severe shortages human resources, medical equipment and training on how to handle the disease. Already tiny, under-equipped clinics couldn’t handle the influx of patients. Sierra Lione had roughly 51 physicians for 5 million people, that’s a 1:98,000 physician to citizen ratio, andprotective equipment was so lacking that people initially had to use plastic bags in place of gloves. Without personal protective equipment, many health workers ended up dying from the disease, leaving less people to care for increasing cases. Countries like America also discouraged volunteering, firing everyone who wanted to help in Africa for fear of them bringing back Ebola, driving down the number of outside helpers even more.
While there were definitely shortages in Wuhan, the first epicenter of COVID-19, China definitely had better resources and medical facilities available for its citizens. Following the outbreak, 23 000 doctors and nurses were mobilized to Hubei Province (Wuhan is the capital of Hubei), that’s a ratio of around 1:2,500 physicians to citizens. Still a crazy stretch, of course (even assuming that not every citizenwill fall sick), but already way, way better than the ratio in Ebola hotspots. China is also much richer than the West Africas, and besides the money the Chinese Government was pouring into the COVID-19 fight, many wealthy Chinese businessmen and celebrities donated millions of dollars worth of medical equipment, masks and money to fund research and treatments.
China had far better capabilities to deal with COVID-19 than the West Africas had with Ebola. Perhaps you could consider Ebola’s high death rate a reflection of the struggling African response, and COVID-19′s lower one a reflection of the more prepared Chinese one. It’s NOT, however, a direct reflection of which diseases is more dangerous on its own and by how much. If COVID-19 had broken out in a country with the same resources as West Africa, the death toll would undoubtedly be much higher.
But that was at the beginning of the outbreak. Now, the situation around the world isn’t looking too great. COVID-19 in over 190 countries, many whose medical systems are sorely under-prepared to handle the virus, placing nations at risk of healthcare collapse. As medical supplies, human resources and hospital beds run out, more people will unquestionably die. The mortality rate has already risen from 2% to 4% since I started writing this article.
C. Infectiousness and Scale of Disease
Miraculously as it seems, Ebola mostly stayed within the African nations with only 14 cases outside (USA-11, Italy-1, Spain-1, UK-1). This was because Guinea, Sierra Leone and Libera (regions most affected) were already fairly isolated nations, and being right next to the sea prevented the virus from spreading in that direction. Local governments set-up strict border control, and international airlines/private companies basically stopped flying to Africa so few people could carry the virus outside affected areas.
While Ebola spreads through direct contact, COVID-19 is spread through droplets that can cling to hard surfaces, making it much more infectious. Despite Hubei’s lockdown, the virus managed to spread to over 190 countries across the world where cases will only continue to rocket unless governments act fast. Just for comparison, yes Ebola killed 50% of cases, but its scope was much smaller with 28,637 cases in contrast to Corona’s 430,000 cases (and counting). COVID-19’s scope is wider than not just Ebola, but also 2003′s SARS (26 countries, 8098 cases) and 2012′s MERS (27 countries, 2494 cases) which it is often compared to.An outbreak of this scale hasn’t been present since the Spanish Flu in 1918 (which affected over 500 million people).
Now how does that translate in terms of danger? Well, with outbreaks focused in few regions like Ebola, it’s much easier to coordinate support from international organizations (MSF, WHO…) and other nations. People know exactly where they should be sending resources and supplies, and where to direct help. But when all 195 countries are infected with the virus, it’s impossible for WHO to help all nations that need it because there just aren’t enough resources! When everyone’s struggling to contain their own cases, helping other countries just isn’t a priority anymore. The world can come together to help 3 countries, maybe even 30, but all 195? That’s a completely different story.
Mini conclusion: Don’t be fooled by COVID-19′s seemingly low mortality rate into thinking it isn’t dangerous. COVID-19 is of larger scale than all recent pandemics, including Ebola, and threatens to bring a bigger danger: the collapse of healthcare systems worldwide. Governments can lower cases and deaths by taking strict preventative measures and ensuring enough resources/supplies are always available at hand.

2. Community Engagement + Trust = Success (well that’s the gist of it, anyway)
A. Community Engagement vs. Individual Satisfaction
In countries like China, Vietnam, South Korea, and recently Italy, governments have taken strict measures to control the virus, including but not limited to cancelling schools and events, issuing detailed quarantine/treatment protocols and educating people of the disease nationwide. Citizens have banded together and are closely cooperating with their government to overcome the epidemic. The Vietnamese Prime Minister has even called the effort “Chống Dịch Như Chống Giặc” which roughly translates to “Fighting the virus like fighting against invaders/enemies.” This is not an exaggeration. With every single person and community fully engaged and playing their part to stop COVID-19, it really does feel like we’re “going to battle.”
Countries with the highest levels of community engagement and strongest government responses have proven to be most successful in dealing with pandemics time and again. They don’t even need the most money or best medical equipment, just complete trust in their government’s efforts and the mindset of everyone doing their part for the greater good.
Interestingly enough, many countries successfully containing COVID-19 are Asian despite being closer to the initial outbreak, which might reflect the emphasis on “community” in Asian cultures, while Western nations that prioritize “individuality” generally end up doing worse. For example, at one time Italy and South Korea both had around 7000 cases, but Italy’s death toll was 366 while South Korea’s was 50. Koreans had shut down schools and public events, issued tens of thousands of tests, and were all self-quarantining. Italy had seen thousands of cases the week before, yet citizens at that time showed little concern and still gathered en-mass, allowing the virus to spread more quickly. This was right before the Italian Government announced COVID-19 as a national emergency and locked down the entire country—only then did people start taking it seriously.
Notice how both situations dealt with viral spreads, but Koreans’ strict abidance to community guidelines early on helped lower the number of fatalities drastically, and now Korea is reporting fewer and fewer new cases every day while Italy’s numbers are still increasing exponentially. Likewise, in America where governments ignored WHO’s emergency warning and failed to take precautionary measures against COVID-19, numbers are soaring with over 30,000 cases accumulating in 3 weeks. Countries where people choose to indulge in short-term individual satisfaction end up facing far worse consequences than countries which choose to sacrifice some personal liberties early on for the greater good.
B. The Problem of Trust
So now let’s talk about trust, another crucial factor in dealing with pandemics. When Ebola hit the West Africas in 2014, one of the biggest hurdles hindering recovery early on was the complete lack of trust between citizens, the government and even international helpers. When physicians from abroad first showed up, they were shunned—locals didn’t trust these strangers in plastic suits and goggles, speaking tongues different from their own. Locals didn’t trust that the healthcare system could actually cure them, and in many districts people stopped going to clinics entirely for fear of contracting Ebola. Imagine the complications that arose because of that lack of trust! People refusing to visit clinics meant more severe infections, more deaths, more transmissions, and lack of cooperation with government efforts.
The early days of Ebola were a medical disaster. It was only when the government solidified trust with citizens by training community health workers and educating nationwide about the disease that things started looking up. Likewise, to successfully control and overcome COVID-19, governments and their citizens must trust each other wholeheartedly and closely cooperate to push back dangers.
“Learn to trust the government if they’re taking action. It’s not because they’re more intelligent or more prepared than you, certainly, but they are the only people with access to all of the available information. Knowledge is power, now more than ever. We are able to evaluate and predict the effect of the measures, so there’s a reason they’ve been taken.” — Angelo Sidonio.
Right now, trust is a big problem. People all over the world are in panic because they don’t believe their governments are doing everything possible to keep them safe. And they’re rightfully concerned! As food banks and shelters close down due to lack of volunteers, over 320,000 homeless people in the UK, unable to self-isolate, face even greater dangers than before. In America, where almost 40 million people live in poverty and another 3 quarters live paycheck to paycheck, sky-high medical bills can either discourage citizens from seeking treatment, or push those who do into bankruptcy. And that’s assuming they even get treated, for although America is taking some measures like “social distancing” only a tiny number of cases are being dealt with. As of March 23rd, Spain and America both have around 30 000 cases, yet Spain has finished treating 4,400 cases while America has only treated 636 — that’s a difference of seven times!
Until governments can prove themselves trustworthy to their citizens, the efforts to contain COVID-19 will be long, arduous and without unanimous support. This means ensuring even the most vulnerable groups feel protected and assuring citizens that should they contract the virus, they will get quality treatment that won’t break the bank. Trust minimizes panic, boosts morale and creates unity, putting the country in a better position to defeat the pandemic.
Mini conclusion: To overcome pandemics 1) Citizens must trust that the government is doing everything possible to protect them (gov. should actually be doing this by the way!) and 2) Everyone must be fiercely involved in community engagement, playing their part to stop the disease spread. Personal sacrifices are sometimes necessary for the greater good. Trust minimizes panic, boosts morale and cooperation.

3. So what can YOU do about all this?
A lot of what I’ve just said points to systematic issues and government decisions that most of us can’t really change (unless you’re perhaps planning to become the next world leader, then yes, please go ahead and change them), so I’ll talk a bit about what we can do as students or individuals. There’s obviously all that stuff about washing your hands and self-quarantining which I won’t repeat—you can access WHO’s guidelines here and Vietnam’s guidelines here—but below are some other important things worth considering:
A. Raising Awareness and Educating Others
In many countries, there has still been no official nationwide efforts to educate the public on the risks of COVID-19, leading to many citizens either misunderstanding, trivializing or being ignorant of the topic. If you live in such an area, do your part by raising awareness on the following points, plus any more you can think of:
“Othering” and Exoticizing
COVID-19 brought about another disease: racism. Across the world, Asians are being shunned, discriminated against and seen as “carriers of the virus.” Many Chinese restaurants are losing customers, and some Asians are even getting beat up for wearing masks.
This is what you would call “othering”—somehow exoticizing COVID-19 as something intrinsically separate and different from oneself. “Oh that’s a Chinese disease that originated from exclusively Chinese practices of eating wild animals! It has nothing to do with me!” Saying this makes people feel “separated” from the risks because they don’t partake in these “distinctively Chinese” practices that lead to COVID-19. This is all false security, though. COVID-19 and its modes of transmission isn’t “distinctly Chinese” and consumption of wild animals is found across the globe (France, America…)
To exoticize human practices as “different” or “savage” is clearly racist and shouldn’t be condoned/ignored under any circumstances. However, do be careful as to how you go about responding to these people. If you’re aggressive, it will most likely backfire. If you can, try to remain calm and build understanding (most of these people are just ignorant, not inherently evil and incapable of love), as attacking them will only make them more defensive. More importantly, check on the victims of racism: let them know you support and stand by them.
“It’s only dangerous in ______! We’re safe here!”
But are you really? In a world as interconnected as ours, is there really such a thing as ‘only local’ anymore? Do you have family members or fellow citizens in epidemic hotspots? With millions of trains, cars and airplanes flying between cities, states and countries, do you really think there’s no chance that the virus will spread to where you currently live? At the start, we all thought COVID-19 could be contained in China, yet now it’s in 190 countries with rocketing numbers! There’s no such thing as completely safe, and many precautions are free and easy.
Trivializing: “It’s not even that dangerous! I’ll go to the pub if I want to! Plane tickets are on sale, so maybe I’ll go travelling too!”
Please don’t be irresponsible. You might not be at risk, but walking around and going to crowded places increases the chance of you picking up the virus and spreading it to others with who won’t survive! Perhaps you’ll end up passing it to your parents, grandparents, or someone with underlying health problems whose infection would be fatal. Perhaps you’ll pass it to someone without health insurance, who can’t pay for the cost of treatment. Remember that it won’t just be you suffering if anything bad happens, but those around you as well.
B. Educate Yourself: Study the Situation In Depth
Next! Other than teaching others the basic know-hows of COVID-19, it’s also important to educate yourself. And I don’t just mean knowing the basic symptoms and 6 steps of hand-washing. Most of us are self-quarantining with not much to do. Go deeper.

If you have the time, study how nations, NGOs and international organizations dealt with past pandemics, which methods succeeded or failed, and how they’re currently dealing with this epidemic. How is funding for research related to infectious diseases allocated and how can we improve the system for information sharing between scientists and nations? How and when does the WHO, World Bank, UNICEF and other UN Institutions allocate funding, humanitarian aid and expert help in a time when demand outweighs supply? What levels of involvement and accountability are to be expected at the level of individuals, communities, nations, and international organizations and how should they work together?
It’s a lot of knowledge, certainly, and you needn’t learn it all at once. But understanding the relationships between public health, economy and politics (even at a very basic level) will be tremendously helpful in making sense of why governments/organizations do what they do, and how our lives will be affected. At the end of this article I’ll list some resources I’ve found valuable for you to check out if you’re interested.
4. What Nations Can Do (Not an Expert Though So Maybe Don’t Quote Me On Your Essay)
Disclaimer: I’m not an expert on this so if someone actually does this and it ends up failing, don’t sue me. But alright, after taking the course on dealing with pandemics and observing how countries around the world are reacting, I’ve pieced together some basic steps that might work.
S. “TEST, TEST, TEST!”
In a press briefing on 16th March 2020, WHO Director General Tedros Adhanom Ghebreyesus announces “We have a simple message for all countries: test, test, test!” He emphasizes testing, isolation and contact-tracing as the backbone of the response, and urges nations to ramp up on these measures. That’s not to say that social distancing isn’t important—it is and we MUST continue to do it —but quarantining alone is not enough to extinguish the pandemic.
South Korea’s success in driving down it’s number of cases from exponential increase to few new cases per day is largely credited to its efficient testing. South Korea has issued over 380,000 tests since the COVID-19 outbreak in its country, and is testing some 20,000 people everyday. By testing suspects or those with mild symptoms, carriers are isolated and treated before they can spread it to others, well before their condition becomes fatal. With the recent donation of testing kits from WHO and other organizations, hopefully many more countries will also see the lowering numbers of this nation.
A. Nationwide Education on Pandemic
Next, to put out the epidemic, countries must provide ongoing, consistent and thorough education to the public about COVID-19 nationwide, regardless of whether they’re epicenters or not. No, a government official going on TV to say 5 sentences about the breakout is not enough.You cancelled classes? All your students should deeply understand why it’s so important that we don’t gather in crowds and spend that time isolating, not gathering at parties to ‘celebrate.’ Instead of the occasional “just wash your hands” reminder, comprehensive hygiene protocols should be put up noticeably everywhere and everyone should be able to repeat them.
Schools, hospitals, companies, communities and families must all have guidelines for dealing with the virus (appropriate to the level of severity in their area), and constantly be reminding their members of these duties.Every individual must deeply understand what they’re dealing with, what the risks are and how they can play their part in fighting the epidemic.
B. Standardized Procedures & Training
To educate, there needs to be standardized guidelines, procedures and protocols to educate with. Perhaps it would wise to train physicians around the country instead of just those at epicenters: that way when new cases arise away from the epicenter, local physicians can treat them right there instead of transporting them to hospitals in other cities, increasing chances of spreading the disease along the way (Vietnam is doing this.) Train community workers too, so they know how to handle local cases and can educate their communities–in an emergency like this, no community must be left ignorant.
For the general public, training on remote working is necessary too: many companies and schools are struggling with effective online meetings and communications. It’s only when everyone’s forced to work online that you realize many teachers don’t know what the heck they’re doing and everyone’s webcam/mike is off because they’re actually looking at memes instead of studying.
C. Strengthening Emergency Responses
Perhaps two months ago this section would be named “improve your healthcare system to prepare for the worst” but now that we’re in the middle of the outbreak, it’s impossible to fix everything as we go along. Instead, right now nations must strengthen their emergency response systems. This means being able to re-allocate funds and human resources to necessary areas, build/transform new treatment/quarantine wards and hospitals quickly, and ensure no shortages of medical (and general) supplies.
To meet demands in dire conditions, this requires governments to think outside outside the box and be resourceful, transforming their current assets (even if lacking) into something usable. In Singapore, this means using the army to pack masks and supplies for the population. In Vietnam, it meant clothing factories switching gears to mass-produce affordable, safe cloth masks to make up for shortages. It could mean governments hiring airlines and restaurants to make food for people in quarantine, transforming army camps or hotels into quarantine wards, quickly finding ways to train new personnel or creating an online health reporting system for their citizens. Whatever the case, an emergency like this one requires governments to step up their game and respond faster.
D. 10 Recommendations for Reform Before The Next Pandemic
To get more onto the academic side of things, after the Ebola outbreak of 2014, the Harvard-LSHTM Independent Panel on Ebola came out with this report, outlining 10 reform recommendations to help deal with future pandemics. I feel like a lot of it is still relevant today and should be adopted by nations to tackle the COVID-19 situation. I will quickly summarize the report in bullet points below because it’s super long, but check it out for yourself if you have time:
Prevention:
- Nations must invest domestically in their core capacities (strengthening healthcare system, education programs…) The global community should provide poorer countries with funding and help to invest in these capacities.
- WHO should promote early reporting of epidemics. There should be financial incentives for countries that report early to 1) Help deal with the outbreak and 2) Compensate for economic losses.
Response:
- WHO should create a Center for Outbreak Response with strong technical capacity, generous budgets and clear accountability lines.
- WHO should create a transparent, politically protected Committee with the power of declaring public health emergencies (right now only the Director General can declare public health emergencies).
- An independent UN Accountability Commission should be created to assess worldwide responses to major disease outbreaks.
Research and Development (R&D):
- Rules/guidelines on operating during/between outbreaks should be developed to oversee efficient research and ensure access to the benefits of research.
- Research funders should establish a worldwide R&D financing facility for outbreak-relevant drugs, vaccines, diagnostics, and non-pharmaceutical supplies.
Governing global system on prevention and response:
- Create a Global Health Commission in the United Nations Security Council (UNSC).
- WHO should focus scale back expansive activities and focus on it’s core functions. In outbreaks, focus on 1) helping nations improve core capacities 2) rapid early response and assessment of outbreaks (including potential emergency declarations) 3) establishing technical norms, standards, and guidance and 4) convening global community to set goals, mobilize resources, and negotiate rules.
- WHO needs to reform to be more effective. Member states should be vocal about choosing a strong, competent leader.
Again, these recommendations were made after WHO’s response to the Ebola outbreak of 2014. Although COVID-19 will bring about many new difficulties not yet covered in this report, it’s still a valuable guide for how we can prepare for the worst. WHO has since carried out multiple reforms, and despite the severity of the situation, are responding faster this time round to provide the world with information to tackle the crisis. Looking at successes to contain the disease around the world, we know what works. If all countries could apply those measures responsibly, we can pull through.
5. Helpful Resources
Lastly, I’d like to share some resources I’ve found tremendously helpful in understanding this COVID-19 ordeal. Check them out when you have time!
First, the “Lessons from Ebola: Preventing the Next Pandemic” online course from Harvard University that I mentioned at the beginning. The course runs for 1 month and is totally free! I got a lot of valuable insight from it on international responses to major infectious outbreaks. Although only Ebola is talked about in specific, a lot of it can apply to other diseases too, and I highly recommend it for basic understanding.
For general information:
- Vietnam’s COVID-19 website from the Ministry of Health
- World Health Organization (WHO) COVID-19 Updates and General Information
- Worldometer (COVID-19 case tracker)
- Interactive Map showing global COVID-19 spread – Johns Hopkins CCSE
- Interactive Map showing global COVID-19 spread – WHO (out of the 3 trackers, Worldometer usually updates fastest)
- This one Mark Manson article on Individual vs. Systematic risks and other risks and biases of COVID-19
- New York Times has good articles for US coverage, CNBC for worldwide-ish coverage, but Western media has a bias against China, so check out South China Morning Post for coverage from the East.
- Ghen Co Vy – A Bop to Wash Your Hands to
Scientific Journals/Sciencey sources to track research reports. While normally many journals charge fees, recently all information regarding COVID-19 has been changed to open-access:
- The Lancet’s COVID-19 Resource Center
- Cell Press COVID-19 Resource Center
- Elsevier COVID-19 Information Center
- The BMJ
- WHO COVID-19 Global Research Database
That’s all I can think off right now! I’ve linked most of my sources in the article, and will provide additional updates to information when I can. For now I hope this article was useful and helped you learn something new about the COVID-19 pandemic, no matter now big or small.
Depending on the situation, our days of self-quarantine can last anywhere from a few weeks to months. In that time, remember to stay vigilant and take necessary precautions to protect yourself and your community, but also stay calm because panicking won’t help. Eat and drink healthily, stay clean and safe, learn things and look out for others. Let’s conquer this virus together!
All statistics are of 25th March 2020 and prior.